Published: May 13, 2026 | Last updated: May 13, 2026
How to Naturally Increase Testosterone: The 4-Lever Protocol Backed by Science
If you want to know how to naturally increase testosterone, you need more than a list of tips. You need to understand the biological machinery that produces it.
Testosterone is not a mood or a mindset. It is a hormone manufactured by a specific assembly line inside your body, and every lifestyle factor in this article either feeds that assembly line or actively blocks it.
Most articles on testosterone optimization stop at "sleep more and lift weights." That is correct, but it explains nothing. Without the mechanism, you will not follow through consistently.
This guide covers the four evidence-backed levers in full: sleep, resistance training, nutrition, and stress management. Each section starts with the biology, then delivers the protocol.
If you want to go deeper on sleep specifically, the evidence-ranked guide to improving sleep quality is the most detailed resource on this site for men who train. The article on building a morning routine that actually sticks covers the circadian anchoring that sets hormone production up from the start of the day.
If you are new to the conversation around physical performance and why it matters, why your body is the most important asset you will ever own is the right starting point. And if you have heard anything about creatine affecting testosterone-related hormones, the full creatine monohydrate breakdown covers what the research actually says.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional before making changes to your diet, exercise, or supplement routine.
Disclosure: This article contains affiliate links. If you click through and make a purchase, I may earn a small commission at no extra cost to you. I only recommend products I genuinely believe in.
Testosterone optimization is the process of maximizing the body's natural production of testosterone through evidence-based lifestyle interventions that support the hypothalamic-pituitary-gonadal (HPG) axis. It matters because testosterone directly governs muscle mass, energy, libido, mood regulation, and long-term metabolic health in men. This guide is built for men aged 25–35 who want the science behind each lever, not a generic wellness checklist.
To naturally increase testosterone, target the four primary biological levers: optimize sleep to 7–9 hours nightly (since most testosterone is produced during slow-wave sleep), perform 3–4 weekly sessions of heavy compound resistance training, consume adequate dietary fat and correct any zinc, magnesium, or vitamin D deficiencies, and actively manage chronic cortisol through structured recovery and stress reduction. Consistent application of all four levers over 8–12 weeks produces measurable changes in testosterone levels for most men.
Quick Takeaways
- One week of 5-hour nights reduces testosterone by 10–15% in healthy men.
- Testosterone is mainly produced during deep sleep, not waking hours.
- Heavy compound lifts (6–10 reps) drive the strongest hormonal training response.
- Dietary fat is the raw material for testosterone – cutting fat cuts hormones.
- Vitamin D deficiency is linked to measurably lower testosterone levels.
- Chronically high cortisol directly suppresses the HPG axis that makes testosterone.
Source: Leproult & Van Cauter, JAMA (2011); Kraemer & Ratamess, Sports Medicine (2005); Pilz et al., Hormone and Metabolic Research (2010)
What Is Testosterone and Why Does It Decline?
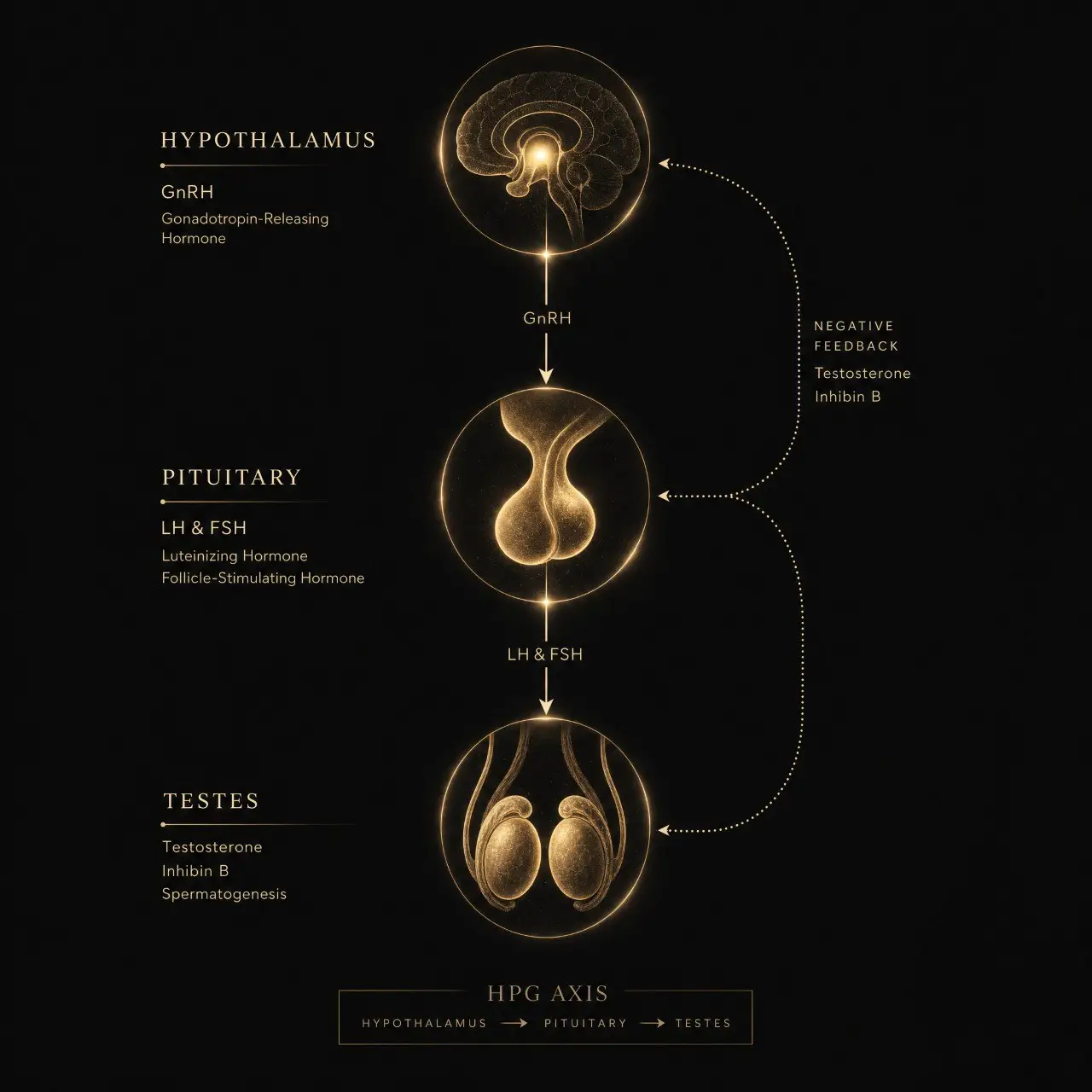
Testosterone is a steroid hormone produced primarily in the Leydig cells of the testes. It is not manufactured on demand. It is released through a precise hormonal relay called the HPG axis (hypothalamic-pituitary-gonadal axis). The hypothalamus releases gonadotropin-releasing hormone (GnRH), which signals the pituitary to release luteinizing hormone (LH), which in turn signals the Leydig cells to synthesize testosterone from cholesterol.
Normal total testosterone in adult men ranges from 300 to 1,000 ng/dL, according to current clinical reference ranges from the NIH's StatPearls testosterone reference guide. For most men in their 20s, the optimal zone sits between 600 and 900 ng/dL. Levels below 300 ng/dL indicate clinical hypogonadism.
The range between "technically normal" and "optimized" is where the majority of men in their 30s quietly lose ground.
Source: Miller & Auchus, Endocrine Reviews (2011) – 2,382 citations; Wang et al., Journal of Clinical Endocrinology & Metabolism (2005)
The 1% Decline: What the Research Actually Shows
After age 30, testosterone declines at roughly 1% per year. Andrew Huberman references this figure in his 2025 Huberman Lab Essentials episode on testosterone and estrogen optimization, drawing from clinical literature. The foundational epidemiological study is Feldman et al. (2002), the Massachusetts Male Aging Study (PMID 11836290), which tracked this decline longitudinally in men aged 40–70.
The rate is gradual enough that most men will not reach clinical hypogonadism from age alone. Even so, the cumulative effect over a decade without intervention is real and measurable.
In practical terms: a man who is at 750 ng/dL at 30 may be at 600 ng/dL by 45 without changes to sleep, training, nutrition, or stress. That difference shows up as reduced energy, slower recovery, lower drive, and harder body composition battles. It is not a dramatic collapse, but a slow erosion.
The good news is that all four levers in this article act on the same axis and can reverse that trajectory without prescription intervention.
Free vs. Total Testosterone: The Number That Actually Matters
Total testosterone includes both bound and free fractions. Most testosterone in the bloodstream is bound to sex hormone-binding globulin (SHBG) or albumin and is biologically inactive. Free testosterone (typically 1–3% of total) is what actually enters cells and drives the effects you care about.
As a result, a man with high total testosterone but elevated SHBG may experience symptoms of low testosterone despite "normal" lab values.
Factors that raise SHBG and reduce free testosterone include excess body fat (aromatase activity converts testosterone to estrogen), chronic alcohol use, and low magnesium. Factors that lower SHBG and improve free testosterone availability include resistance training, adequate zinc, and weight loss. This is why the 4-lever protocol works on both total testosterone production and on the availability of the testosterone already being produced.
Sleep: The Single Most Powerful Natural Testosterone Lever
Sleep is the foundation of testosterone production, not a supporting factor. The majority of daily testosterone secretion occurs during sleep, tightly coupled with slow-wave (deep) sleep architecture.
If your sleep is short, fragmented, or shallow, you are not just tired. You are cutting your body's primary testosterone production window.
What the Research Shows: The JAMA Sleep Study
The clearest evidence comes from a landmark 2011 study by Leproult and Van Cauter, published in JAMA. They took healthy young men aged 24.3 ± 2.8 years and restricted their sleep to five hours per night for one week. The result: daytime testosterone levels dropped by 10–15% compared to baseline. The drop was concentrated in the afternoon, the window when men typically report the lowest energy and motivation.
Five hours of sleep is not unusual for working men in their late 20s and 30s. The CDC's National Center for Health Statistics reports that more than one-third of U.S. adults regularly sleep fewer than seven hours per night, and that proportion is higher among working-age men. The Leproult study makes the causal link explicit: less sleep means less testosterone, measurably, within days.
The Mechanism: Why Sleep Is the Production Window
Testosterone release follows a circadian pattern. LH is secreted in pulses during sleep, stimulating Leydig cell activity in the early hours of the night and peaking during slow-wave sleep. Research published in the Journal of Neuroscience (Mong et al., 2011) confirmed that slow-wave sleep directly supports gonadal function and cell turnover in reproductive tissue. Disrupting sleep architecture through late nights, alcohol, blue light exposure, or fragmented sleep cuts both total sleep time and the proportion of slow-wave sleep, the specific phase where testosterone production peaks.
"Going into deep sleep and getting the proper patterns of slow-wave sleep and REM sleep are important for hormone optimization. Deep sleep supports the gonads, the ovaries and the testicles, and the turnover of cells and the production of cells."
– Andrew Huberman, Neuroscientist, Stanford School of Medicine
The Sleep Protocol for Testosterone Optimization
Target 7–9 hours of uninterrupted sleep in a cool, dark room. Anchor your wake time to a fixed hour, even on weekends, to stabilize the circadian rhythm that governs LH pulsatility. Avoid alcohol within three hours of bedtime; even moderate alcohol suppresses slow-wave sleep architecture without reducing total sleep time, meaning you sleep but do not recover. For the full evidence-ranked sleep protocol, the sleep quality guide for men who train on this site covers every intervention tier.
Resistance Training: How Exercise Drives Testosterone Naturally
Heavy resistance training is the most direct training stimulus for testosterone elevation among men. The acute post-exercise testosterone spike contributes to the chronic adaptation that keeps baseline levels elevated over time. The training variables matter, though. Not all exercise produces the same hormonal response.
What the Research Shows: Kraemer and Ratamess (2005)
The definitive reference on this topic is the review by Kraemer and Ratamess, published in Sports Medicine (2005), a paper with over 1,363 citations. Their analysis established the key variables: heavy multi-joint movements (squats, deadlifts, rows, presses), moderate-to-high volume (4–6 sets), loads at 70–85% of 1RM in the 6–10 rep range, and short rest intervals of 60–90 seconds between sets produce the greatest acute testosterone response.
Large muscle mass recruitment is the driver. The more total muscle tissue involved, the stronger the hormonal signal.
The acute spike is transient: 30 to 60 minutes. The chronic adaptation is what matters for testosterone optimization. Men who train consistently with heavy compound movements maintain higher baseline testosterone compared to sedentary men or those training with low loads. The HPG axis adapts upward in response to the cumulative hormonal signal.
The Testosterone:Cortisol Ratio: A Trackable Training Marker
Sports scientists use the testosterone-to-cortisol (T:C) ratio as a marker of training state. When this ratio is favorable, recovery is efficient and performance improves. When cortisol chronically dominates through overtraining, insufficient recovery, or high-volume low-intensity work without adequate rest, the ratio inverts, testosterone drops, and training progress stalls. This is why training frequency matters as much as training intensity: 3–4 heavy sessions per week with full recovery days outperforms 6–7 sessions per week in terms of hormonal outcomes for most men.
The Training Protocol for Testosterone Optimization
Structure your training around multi-joint compound movements: squats, deadlifts, Romanian deadlifts, barbell rows, bench press, and overhead press. Train each major muscle group 2x per week with 4–5 sets per movement in the 6–10 rep range at 70–85% of your 1RM. Keep rest intervals at 60–90 seconds. Limit weekly training sessions to 3–4 to maintain a healthy T:C ratio. Cardio is fine, but excessive endurance volume (more than 5 hours per week) chronically elevates cortisol and blunts testosterone response in men not specifically conditioned for it.
The Nutrition Protocol for Higher Testosterone
Testosterone is biosynthesized from cholesterol. Leydig cells require cholesterol as the raw substrate for the steroidogenesis pathway, and cholesterol availability is directly influenced by dietary fat intake. If your nutrition does not support this substrate, the assembly line stalls regardless of how well you sleep or train. This section covers the three most evidence-supported nutritional levers: dietary fat, zinc, and vitamin D.
Dietary Fat: The Raw Material for Testosterone Production
The most overlooked finding in testosterone research is the direct relationship between dietary fat intake and androgen levels. A controlled trial by Wang et al., published in the Journal of Clinical Endocrinology and Metabolism (2005), found that switching middle-aged men from a high-fat to a low-fat, high-fiber diet reduced circulating androgen levels by 12%, without changing caloric intake or activity levels. The mechanism is straightforward: less dietary fat means less available cholesterol, which means reduced substrate for Leydig cell steroidogenesis.
Men who follow very low-fat diets during aggressive caloric cuts are actively suppressing their testosterone substrate. In practice, this means keeping dietary fat at 25–35% of total caloric intake. Prioritize sources high in saturated and monounsaturated fat: eggs, red meat, olive oil, avocados, and nuts.
These are not empty calories. They are the building materials for the hormone you are trying to optimize.
Zinc: The Cofactor That LH Receptor Function Depends On
Zinc is a required cofactor for LH receptor function and for multiple enzymes in the testosterone biosynthesis pathway. A 1992 study by Hunt, Johnson, and Herbel in the American Journal of Clinical Nutrition showed that dietary zinc depletion in young men significantly reduced serum testosterone. Zinc deficiency is a direct biological bottleneck for testosterone production.
Zinc deficiency is more widespread than most men realize, particularly in those who sweat heavily during training (zinc is lost through sweat) or who eat low-meat diets. The recommended daily intake for adult men is 11 mg. Food sources include oysters (the highest natural source), red meat, pumpkin seeds, and eggs. If whole-food intake is insufficient, zinc bisglycinate or zinc picolinate are the best-absorbed supplement forms.
Vitamin D: The RCT Evidence for Testosterone Increase
The strongest direct evidence for a micronutrient-testosterone link comes from a randomized, placebo-controlled trial by Pilz et al., published in Hormone and Metabolic Research (2010). In men with vitamin D deficiency, supplementing 3,332 IU of vitamin D daily for one year increased total testosterone from 10.7 to 13.4 nmol/L, a roughly 25% increase. Free testosterone and bioavailable testosterone also increased significantly. The placebo group showed no change.
One caveat: this effect was demonstrated in vitamin-D-deficient men. Supplementing in men who are already sufficient may produce a smaller benefit. Given that vitamin D deficiency is estimated to affect 24–41% of U.S. adults (Forrest and Stuhldreher, Nutrition Research, 2011, PMID 21310306), testing 25(OH)D serum levels before supplementing is worthwhile. The target range for testosterone optimization is 40–60 ng/mL. Standard supplementation doses range from 2,000–4,000 IU daily depending on deficiency severity and sun exposure.

Magnesium: The SHBG Reducer
Magnesium supports testosterone optimization through a different pathway than zinc. Higher magnesium levels are associated with lower SHBG, which means more free testosterone from the same total testosterone production. Magnesium also improves sleep quality by supporting the GABAergic system that drives slow-wave sleep, providing an indirect testosterone benefit through the sleep lever. Dietary sources include dark leafy greens, pumpkin seeds, dark chocolate, and legumes. Magnesium glycinate or Life Extension Neuro-Mag Magnesium L-Threonate are well-tolerated supplement forms.
A Note on Creatine and DHT
A single small study (van der Merwe et al., 2009, n=20) found that creatine supplementation increased the DHT-to-testosterone ratio in young rugby players, suggesting a potential effect on the conversion of testosterone to its more potent form, dihydrotestosterone. This finding has not been consistently replicated and should not be treated as an established mechanism. For a thorough breakdown of what creatine actually does and does not do, the full creatine monohydrate guide on this site covers the evidence in detail. If you decide to add creatine to your protocol, Nutricost Creatine Monohydrate is a well-dosed, clean-label option.
How Cortisol Destroys Testosterone – and How to Fix It
Cortisol and testosterone are produced through the same steroidogenesis pathway, using cholesterol as a shared precursor. When the body is under chronic stress, the HPA axis (hypothalamic-pituitary-adrenal axis) prioritizes cortisol production. The result is a direct competition for the same biochemical substrate, and under chronic stress, cortisol wins.
The HPA-HPG Antagonism
Beyond substrate competition, cortisol suppresses GnRH release at the hypothalamus, the first step of the HPG axis. Less GnRH means less LH, which means less signal to the Leydig cells to produce testosterone. Chronic psychological stress, sleep restriction (which also elevates cortisol), overtraining, and severe caloric deficits all activate the HPA axis and initiate this suppression cascade.
"Testosterone has this incredible effect of making effort feel good. Testosterone lowers stress and anxiety in males."
– Andrew Huberman, Huberman Lab Essentials (2025)
The relationship is bidirectional: low testosterone increases stress sensitivity, and chronic stress further suppresses testosterone.
Ashwagandha: The Adaptogen With the Strongest Cortisol Evidence
Among supplements with cortisol-lowering effects, ashwagandha (Withania somnifera) has the strongest clinical backing. A 2023 systematic review by Della Porta, Maier, and Cazzola in Nutrients analyzed nine randomized controlled trials and found consistent cortisol reduction in stressed individuals, with no significant adverse effects in short-term use lasting 30 to 112 days.
The testosterone benefit of ashwagandha is indirect. By lowering chronic cortisol, it removes a primary suppressor of the HPG axis. This is not a testosterone booster in the direct sense. It removes a hormonal brake.
The Stress Protocol for Testosterone Optimization
Managing chronic cortisol requires behavioral intervention, not just supplementation. Practical levers include: establishing a consistent sleep and wake schedule (the most powerful circadian cortisol regulator), limiting training sessions above 90 minutes (beyond which cortisol climbs sharply and testosterone drops), incorporating deliberate rest and recovery days, and reducing chronic psychological stressors through structured daily anchors like morning routines. The morning routine framework on this site is built around exactly this principle, using the first hour of the day to set the hormonal and psychological baseline for everything that follows.
What Does Not Work: Common Mistakes to Avoid
Understanding how to naturally increase testosterone also means knowing what wastes your time and what actively makes things worse. Several common approaches either lack evidence, target the wrong mechanism, or create the opposite of the intended effect.
Mistake 1: Commercial Testosterone Booster Supplements
The vast majority of products marketed as "testosterone boosters" lack clinical evidence for meaningful testosterone elevation in healthy men. Some contain zinc and vitamin D, which work but only in men who are deficient, and are far cheaper to buy as standalone supplements. Others contain compounds with no peer-reviewed human evidence at relevant doses.
The strategy of "taking a test booster" without addressing sleep, training, nutrition, and cortisol is like replacing a fuse in a car that has no engine.
Mistake 2: Overtraining
More training is not always better for testosterone. The testosterone:cortisol ratio is a real physiological variable, and chronic overtraining inverts it. Men who train twice daily, or who add excessive cardio volume on top of heavy resistance sessions without adequate recovery, often see testosterone decline rather than increase. Resistance training works for testosterone when it is performed at the right intensity with enough recovery. Volume beyond that threshold is counterproductive.
Mistake 3: Very Low-Fat Dieting
As covered in the Nutrition section, dietary fat is the raw material for testosterone biosynthesis. Men who eat below 20% of calories from fat during aggressive cuts are consistently found to have lower androgen levels. This is particularly relevant during the popular "cut" phases of body composition training, where fat intake is often slashed. Maintaining fat intake at 25–35% of total calories protects testosterone substrate even in a caloric deficit.
Mistake 4: Ignoring Sleep to Train More
Trading sleep for extra training sessions is one of the worst trades in terms of testosterone. The Leproult JAMA study is clear: one week of five-hour nights reduces testosterone by 10–15%. No additional training session produces a comparable positive benefit. If the choice is between a sixth training day and seven hours of sleep, sleep wins every time for hormone optimization purposes.
Mistake 5: Endocrine-Disrupting Chemicals
BPA and phthalates, compounds found in plastic food containers, plastic water bottles, and processed food packaging, have endocrine-disrupting properties documented in the Endocrine Society's scientific statements on endocrine-disrupting chemicals. They interact with steroid hormone receptor systems and have been associated in epidemiological research – including urinary biomarker studies from the NHANES cohort – with lower testosterone and altered SHBG levels in men. Practical mitigation is straightforward: use glass or stainless containers for food and beverages, avoid heating food in plastic, and reduce processed food consumption. This is not a primary lever but it is a genuine background variable worth addressing once the foundation is in place.
The 4-Lever Protocol: Putting It All Together
The 4-lever protocol is not a supplement stack or a 30-day challenge. It is a set of sustainable systems applied in parallel, each one reinforcing the others. Sleep improves recovery from training. Training reduces cortisol sensitivity. Nutrition provides the substrate that sleep and training need. Stress management protects the axis that all three levers feed. The compounding effect is what produces meaningful testosterone change.
Week 1–4: Audit and Foundation
In the first month, focus on the two highest-leverage inputs: sleep and nutrition. Target 7.5–9 hours nightly with a fixed wake time. Remove alcohol for at least three weeks to restore slow-wave sleep architecture. Increase dietary fat to 25–35% of total calories if currently below that threshold. Get bloodwork done if possible: test total testosterone, free testosterone, SHBG, vitamin D (25-OH), zinc, and magnesium. This baseline shapes the rest of the protocol.
Week 5–12: Build the Training Stimulus
Once sleep is stabilized, introduce or restructure resistance training. Start with 3 sessions per week of compound movements (squat, deadlift, row, press) in the 6–10 rep range at moderate-to-high loads. Progress weekly. Add a fourth session around week 8–10 when recovery is solid. The acute testosterone response from training begins immediately. Chronic baseline elevation becomes measurable over 8–12 weeks of consistent stimulus, per Kraemer and Ratamess (2005).
Week 12 and Beyond: Correct Deficiencies and Maintain
At 12 weeks, re-test if bloodwork was done at baseline. Address any confirmed deficiencies: vitamin D (2,000–4,000 IU daily if deficient), zinc (11–30 mg daily from food and supplement combined), magnesium glycinate (200–400 mg nightly). If cortisol management remains challenging despite behavioral changes, ashwagandha at 300–600 mg of a standardized extract (KSM-66 or Sensoril form) has consistent evidence for cortisol reduction in stressed individuals. These supplements are not testosterone boosters. They are deficiency correctors and cortisol modulators. The foundation is always sleep, training, and nutrition.
4-Lever Comparison: Evidence Tier, Effort, and Timeline
Sleep
- Evidence Tier: Tier 1 – strongest single lever
- Primary Mechanism: Slow-wave sleep drives Leydig cell LH response
- Time to Results: Days (10–15% drop within 1 week of restriction)
- Effort Level: Behavioral – habit discipline required
- Key Study: Leproult & Van Cauter, JAMA (2011)
- Biggest Mistake: Sacrificing sleep for extra training sessions
Resistance Training
- Evidence Tier: Tier 1 – consistent acute and chronic response
- Primary Mechanism: HPG axis stimulation via large-muscle compound movements
- Time to Results: 8–12 weeks for measurable baseline change
- Effort Level: High – 3–4 weekly sessions at 70–85% 1RM
- Key Study: Kraemer & Ratamess, Sports Medicine (2005)
- Biggest Mistake: Overtraining – too much volume inverts the T:C ratio
Nutrition
- Evidence Tier: Tier 1 for deficiency correction; Tier 2 for general intake
- Primary Mechanism: Cholesterol substrate for steroidogenesis; zinc/Vit D cofactors
- Time to Results: 3–12 months (vitamin D); days (dietary fat changes)
- Effort Level: Moderate – dietary audit and targeted supplementation
- Key Studies: Wang et al. JCEM (2005); Pilz et al. HMR (2010); Hunt et al. AJCN (1992)
- Biggest Mistake: Very low-fat dieting during caloric cuts
Stress / Cortisol Management
- Evidence Tier: Tier 1 (HPA-HPG antagonism is well-documented)
- Primary Mechanism: Cortisol suppresses GnRH and competes for cholesterol substrate
- Time to Results: Weeks – cortisol is acutely responsive to behavioral change
- Effort Level: Moderate – behavioral and structural changes required
- Key Study: Della Porta et al., Nutrients (2023) for ashwagandha RCTs
- Biggest Mistake: Using supplements to manage stress while keeping chronic stressors in place
Source: Leproult & Van Cauter, JAMA (2011); Kraemer & Ratamess, Sports Medicine (2005); Pilz et al., Hormone and Metabolic Research (2010); Hunt et al., AJCN (1992)
Frequently Asked Questions
How long does it take to naturally increase testosterone?
The timeline to naturally increase testosterone depends on which lever you address first. Sleep improvements begin affecting testosterone within days – the Leproult study showed measurable decline within one week of restriction, which means the reverse is equally fast. Resistance training adaptations build over 8–12 weeks of consistent heavy training.
Vitamin D supplementation for deficiency correction typically shows effects over 3–12 months. Dietary fat changes produce quicker results, often within weeks, as the cholesterol substrate for steroidogenesis becomes more available.
What are the signs of low testosterone in men?
Common signs of low testosterone in men include persistent fatigue that does not resolve with rest, reduced libido, difficulty building or maintaining muscle mass despite consistent training, increased body fat particularly around the abdomen, lower mood and reduced competitive drive, and slower recovery from exercise. These signs overlap with many other conditions, so bloodwork is the only reliable way to confirm low testosterone as the cause.
Can you naturally increase testosterone after 30?
Yes. While testosterone does decline gradually after 30 at roughly 1% per year (Feldman et al., 2002), this is not a fixed biological ceiling. It is a baseline rate in the absence of intervention.
Men who want to naturally increase testosterone after 30 should consistently optimize sleep, train with heavy compound movements, eat adequate fat and correct micronutrient deficiencies, and manage cortisol. This approach can maintain testosterone levels well within the optimal range through their 30s and into their 40s.
The goal is not to reverse aging. It is to prevent preventable decline.
Does lifting weights increase testosterone?
Yes – resistance training reliably elevates testosterone both acutely (in the 30–60 minutes after a session) and chronically (as a sustained baseline adaptation over weeks and months). However, the training variables matter. Compound movements at high loads (70–85% of 1RM) in the 6–10 rep range with short rest intervals produce the strongest hormonal response, according to Kraemer and Ratamess (2005).
Light isolation work does not produce the same effect.
What foods boost testosterone naturally?
Foods that support testosterone production are those rich in healthy fats and key micronutrients. Eggs, red meat, olive oil, avocados, and nuts provide the dietary fat and cholesterol substrate for steroidogenesis. Oysters, pumpkin seeds, and beef contain high levels of zinc.
Fatty fish like salmon provide vitamin D and omega-3 fatty acids. There is no single "testosterone superfood" – the goal is consistent intake of these categories as part of a diet that keeps fat at 25–35% of total calories.
Does sleep affect testosterone levels?
Sleep is the single most powerful lever if you want to naturally increase testosterone. Most testosterone is secreted during slow-wave (deep) sleep, not during waking hours. The Leproult and Van Cauter JAMA study showed that restricting sleep to five hours for one week reduced daytime testosterone by 10–15% in healthy young men.
This is not a marginal effect. It is equivalent to a decade of age-related decline compressed into seven days.
Is vitamin D a testosterone booster?
Vitamin D supports testosterone production in men who are deficient, which describes 24–41% of U.S. adults according to Forrest and Stuhldreher (2011). The Pilz et al. RCT showed a 25% increase in total testosterone over 12 months of supplementation in deficient men. In men who are already vitamin D-sufficient, the benefit is likely smaller.
Test your 25(OH)D serum levels first – supplementing into sufficiency is the evidence-backed use case.
Does stress lower testosterone?
Yes. Chronic stress elevates cortisol, which competes with testosterone for the same cholesterol precursor in the steroidogenesis pathway and suppresses GnRH release at the hypothalamus – the first step in the HPG axis. The effect is direct and biochemical, not psychological.
Managing chronic cortisol through behavioral structure, adequate sleep, and controlled training volume protects testosterone at the axis level.
What is the normal testosterone range for men?
According to the NIH StatPearls clinical reference, normal total testosterone for adult men ranges from 300 to 1,000 ng/dL. The optimal zone for most men in their 20s and early 30s is 600–900 ng/dL. Levels below 300 ng/dL indicate clinical hypogonadism.
Free testosterone – typically 1–3% of total – is the biologically active fraction and is worth testing alongside total testosterone, particularly if symptoms persist despite normal total levels.
Do testosterone booster supplements actually work?
Most commercial testosterone booster supplements lack clinical evidence for meaningful testosterone elevation in healthy men. The exceptions are the individual components – zinc and vitamin D – which are effective when correcting confirmed deficiencies. These are far cheaper to buy as standalone supplements than bundled in a "booster" product.
No supplement replaces the foundation. If the goal is to naturally increase testosterone, sleep, training, dietary fat, and micronutrient sufficiency are the levers that the evidence actually supports.
How does overtraining affect testosterone levels?
Overtraining chronically elevates cortisol and suppresses the testosterone:cortisol ratio. In men training at excessive volumes – more than four intense sessions per week without adequate recovery, or excessive endurance volume stacked on resistance training – the HPA axis stays elevated, cortisol competes with testosterone synthesis, and baseline levels drop rather than rise. Three to four well-recovered heavy training sessions per week consistently outperforms daily training for testosterone optimization in men who are not elite-conditioned athletes.
Can weight loss increase testosterone?
Yes, particularly in men who carry excess body fat. Adipose tissue contains high aromatase activity, which converts testosterone to estrogen and reduces total testosterone levels. Moderate obesity also depresses SHBG, reducing free testosterone availability.
Weight loss (particularly fat mass reduction through a combination of resistance training and a modest caloric deficit) reverses both mechanisms. However, very aggressive caloric cuts with very low fat intake simultaneously suppress testosterone substrate. A sustainable deficit with maintained fat intake protects testosterone during a weight-loss phase.
How I Know This
I spent three years training six days a week under the guidance of a close friend who served as a marine. That experience was not casual fitness. It was a structured, high-demand protocol built around compound barbell movements, consistent sleep, and nutrition that actually matched the training load.
At peak, I was at 190 pounds, six feet one inch, and under 10% body fat. That outcome was not from supplements or genetic luck. It came from taking sleep seriously, building the training around squat and deadlift variations, eating enough fat and protein to support the volume, and managing recovery the way someone who has been through physical selection manages it – methodically, not randomly.
The research in this article maps directly to what I experienced in practice. The correlation between sleep quality and training performance – and by extension recovery and body composition – was obvious even before I read the Leproult study. The dietary fat point was something I learned the hard way during a poorly-structured cut phase, before understanding the steroidogenesis mechanism.
This article is the article I needed then.
The Bottom Line
Knowing how to naturally increase testosterone comes down to this: testosterone is not a supplement you add. It is a hormone your body produces through a biological assembly line that requires sleep, mechanical loading, adequate nutritional substrate, and a cortisol environment that does not constantly jam the signal.
Most men who feel low on energy, drive, and physical performance are not suffering from a medical condition. They are running the assembly line on inadequate inputs.
The 4-lever protocol is not complex. Sleep 7–9 hours on a fixed schedule. Train with heavy compound movements 3–4 times per week.
Eat enough fat and correct any zinc, magnesium, or vitamin D deficiencies. Manage cortisol through behavioral structure rather than hoping supplements will compensate for a chaotic schedule. Apply all four levers consistently for 12 weeks and measure the result.
Your body is the foundation that everything else in your life runs on – your work capacity, your focus, your resilience, your long-term health trajectory. Testosterone optimization is not vanity. It is infrastructure maintenance for the most important asset you have.
If this article was useful, the guide on why your body is the most important asset you will ever own makes the full case for why treating your body as a serious investment is worth more than almost anything else you could prioritize.
Continue Reading
Randal | Break The Ordinary
I'm Randal, the founder of Break The Ordinary, a multi-niche media brand covering business, tech, health, and finance for people who want to build wealth, freedom, and a life worth living. I spent three years training six days a week under a marine veteran's guidance, reaching sub-10% body fat at 190 lbs, which gave me direct experience with every lever covered in this article. I share what actually works, what doesn't, and what most people get wrong. My approach is direct, research-backed, and built on real experience, not theory.
